This article originally appeared at Your Local Epidemiologist New York. Sign up for the YLE NY newsletter here. Public health, explained: Sign up to receive Healthbeat’s free New York City newsletter here.
Before we begin, I want to touch on some news we received late Wednesday — Centers for Disease Control and Prevention Director Dr. Susan Monarez was abruptly removed, just weeks after the Senate swore her in. Immediately following, three of CDC’s most senior leaders (Drs. Deb Houry, Daniel Jernigan, and Demetre Daskalakis) resigned in protest, citing increased political interference. (You can read Demetre’s powerful resignation letter here.)

This type of leadership implosion at the CDC is not normal. And it definitely widens the vacuum in federal public health guidance that’s been growing over the past year. This instability at our nation’s top public health agency should concern us all. It raises questions about whom we should turn to in the face of health threats, whether it’s seasonal respiratory viruses or the next pandemic. I’m still wrapping my head around this, but I’ll be back with updates as it further unfolds.
For now, let’s get back to this week’s dose.
It’s peak bug season and Covid-19, measles, and mosquitoes are thriving across the state. But it’s not just the bugs: Recent events, from a tragic bus crash in upstate New York to the close of a Legionnaires’ outbreak, show how fragile our systems can be, and how directly that fragility impacts our health.
Here’s what you need to know this week.
Covid-19 ‘weather report’ and an update on fall vaccine availability and FDA approval
All regions of New York show that Covid-19 hospitalizations are elevated. Hospitalizations are still substantially lower than they were this time last year, but are increasing. Given what’s happening in other states, like Florida and Hawaii, we expect increases to continue.
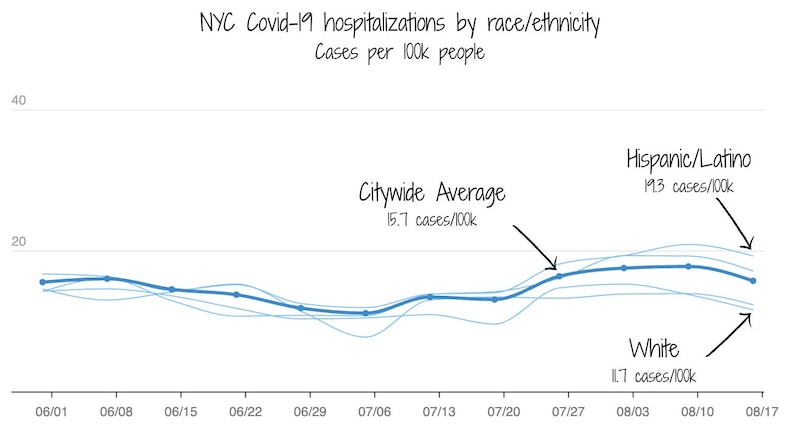
Risk is not spread evenly, and these groups are seeing the highest rates of hospitalization:
- Central New York and the Finger Lakes have the highest rates, when adjusting for population.
- 75 and older age group has higher rates according to data we have in New York City. (We expect it to be the same elsewhere.)
- Hispanic and Latino people have about twice the rate of hospitalization compared to white people. This likely reflects longstanding structural inequities, including greater exposure to risk (from factors such as relying on public transportation or working in more public-facing jobs), more crowded housing, and limitations in health care access, rather than differences in underlying health alone.
What does this mean for you? The best thing to do is wear a mask in crowded indoor areas. I’m going to wear one on the train and at the airport, for example. The Food and Drug Administration just approved fall Covid-19 vaccines, with some significant changes to who will be eligible. YLE National answered several questions on fall Covid-19 vaccines here.
Reflections on the Legionnaires’ outbreak
First, the good news: the Legionnaires’ outbreak in Central Harlem is ending, with fewer and fewer cases being reported after the identification of contaminated cooling towers.
Now, the bad news: Rarely in public health is something random. This outbreak revealed deep cracks in prevention systems in the area:
- Cooling tower monitoring. As I explained a few weeks ago, building owners are legally required to test cooling towers for Legionella every 90 days, and the city aims to inspect each tower at least once per year. But, according to Gothamist, most towers linked to this outbreak were behind on testing and hadn’t been inspected by the city in over a year. And despite increases in funding, the number of inspectors has dropped by more than 30% over the past three years. Enforcement and staffing need attention.
- Health equity. Central Harlem, a predominantly low-income and Black neighborhood, has high risk factors for Legionnaires’ disease among residents, like asthma and diabetes. The city should prioritize enforcement and staffing of inspections in Central Harlem and the surrounding areas, in particular.
- Climate change. Legionella bacteria thrive in warm climates. We should expect Legionella to become more common with climate change and plan accordingly to stay ahead of it.
- Risk communication. In the posts where I covered this outbreak, I tried to communicate that risk was low for most people. However, risk is unevenly distributed, and local communications about the outbreak fell short. Many in Central Harlem feared leaving their homes, and workers said they weren’t given adequate info to keep them healthy. We need timely and transparent communication, including guidance for those at greatest risk, that is grounded in trust and not just broad reassurance.
An outbreak of this size signals that the system failed somewhere upstream. Six people died, and dozens were hospitalized. Everyone deserves to step outside and breathe clean air without fear, regardless of ZIP code.
Mosquito-borne threats: malaria and West Nile
New Jersey, in partnership with the CDC, is investigating a case of malaria in a Morris County resident who may have been infected locally — the patient had not traveled internationally.
For local transmission to occur, two conditions must be met: 1. the right mosquito species (Anopheles), which is commonly found in New Jersey, New York, and most other states, and 2. the malaria parasite itself, which is usually absent here.
If confirmed, this would be big news. Every year, New Jersey reports around 100 malaria cases, almost all among travelers returning from abroad. The last time the state saw a locally acquired case was in 1988. The risk to the public is very low, but public health officials are likely moving quickly to test mosquitoes, treat the patient, and prevent any spread.
The results of mosquito testing will tell us if any local mosquitoes are positive for malaria, but the bottom line is that risk is very low. The best thing you can do is avoid mosquito bites:
- Wear repellent (DEET, picaridin), especially at dawn and dusk.
- Wear long sleeves.
- Dump standing water around your home.
Conveniently, the same recommendations apply for preventing West Nile virus. On that note, the first two human cases of West Nile virus in New York City this year were detected in Queens last week. Now’s the time to break out that repellent!
Tragic Erie bus accident and blood supply
On Aug. 22, a tour bus returning from Niagara Falls overturned on Interstate 90 near Pembroke, killing five adults and injuring dozens. Hospitals quickly drew on local blood supplies, prompting ConnectLife, the area’s primary blood bank serving Erie County Medical Center and Kaleida Health hospitals, to issue an emergency appeal for blood donations.
Smaller cities often lack the blood reserve capacity of large, urban centers. This means mass casualty events can drain the supply overnight, especially for rare blood types or platelets, which have shorter shelf lives. While the emergency need for blood following this accident has likely passed, it’s a sobering reminder that routine blood donations are critical for ensuring readiness for unexpected medical crises.
Here’s where you can donate blood:
- New York City: New York Blood Center.
- Rest of New York state: American Red Cross Blood Donation Centers.
Measles in New Jersey
The New Jersey health department confirmed a measles case in Hudson County, linked to contact with a case from outside the state. Key details remain unclear:
- Did the exposure/transmission occur in a public place?
- Was the non-N.J. resident case associated with international travel or the result of domestic transmission?
- Was either patient vaccinated?
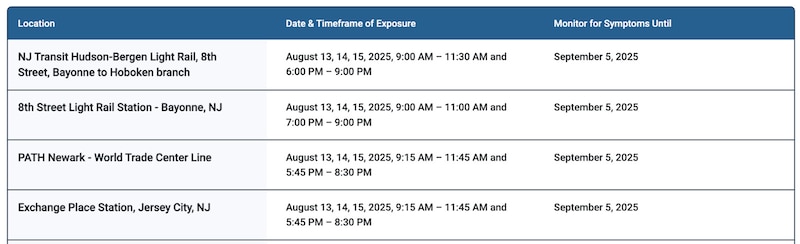
What we do know: The Hudson County case rode PATH and the light rail during commuting hours while potentially infectious. Anyone on those routes may have been exposed. If you are fully vaccinated for measles, you are well protected. If you develop symptoms, contact your health care provider before arriving in person at the doctor’s office.
What else to know this week
Coming up: Free back-to-school vaccine clinics in Buffalo
The Erie County Department of Health is partnering with the University of Buffalo School of Nursing to provide free back-to-school vaccine clinics for Buffalo public school students. These free clinics are taking place as follows:
- Sept. 12, 10 a.m.-2 p.m. at the Buffalo Public School 95 Waterfront, 95 Fourth St.
- Sept. 18, 2 p.m.-6 p.m. at the Buffalo Public School 309 East Community High School, 820 Northampton.
- Sept. 19, 2 p.m.-6 p.m. at the Buffalo Public School 363/415 Lewis J. Bennett/Middle Early College, 2885 Main St.
The vaccines offered include all required school immunizations: DTap/DTP/Tdap/Td; polio; MMR, hepatitis B, varicella, meningococcal, Hib, and PCV (pneumococcal). Students must be up to date on vaccines by Sept. 17 to remain in school, as required by New York State Public Health Law 2164.
Register here for a clinic, and fill out consent forms here.
Bottom line
From Covid and measles to malaria, Legionnaires’, and even blood shortages, this week’s headlines share a theme: Local preparedness matters. Global diseases, chronic inequities, and unexpected crises all land in our neighborhoods. Staying healthy depends on how much our systems — and our communities — are ready to respond.
Love,
Your NY Epi
Dr. Marisa Donnelly, PhD, is an epidemiologist, science communicator, and public health advocate. She specializes in infectious diseases, outbreak response, and emerging health threats. She has led multiple outbreak investigations at the California Department of Public Health and served as an Epidemic Intelligence Service Officer at the Centers for Disease Control and Prevention. Donnelly is also an epidemiologist at Biobot Analytics, where she works at the forefront of wastewater-based disease surveillance.






