Public health, explained: Sign up to receive Healthbeat’s Global Checkup in your inbox a day early.
Hello from Nairobi.
This week’s news is heavy on drug trials and some groundbreaking scientific research – two subjects I try to cover cautiously, because scientists, research institutions, and others have incentives to hype early findings. Anyhow, in global health terms, it is a good issue to be grappling with. It means there wasn’t some new outbreak I had to research.
My name is William Herkewitz, and I’m a journalist based in Nairobi, Kenya. This is the Global Health Checkup, where I highlight some of the week’s most important stories on outbreaks, medicine, science, and survival from around the world.
With that, as we say in Swahili: karibu katika habari — welcome to the news.
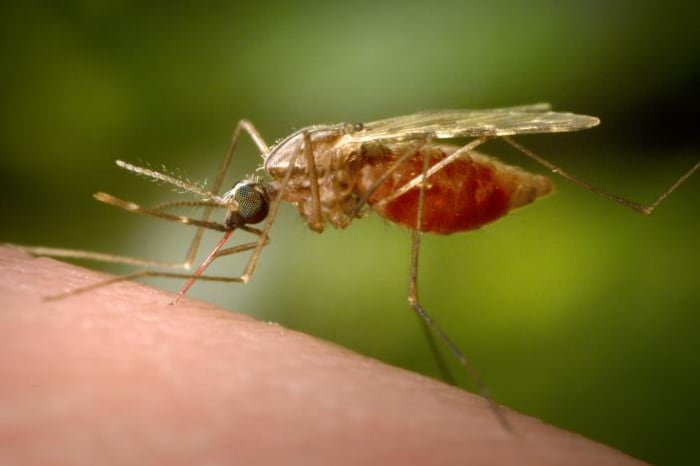
Mainland Europe: a mosquito’s tropical getaway?
There’s a whole rogues gallery of tropical, mosquito-borne diseases that have long been relegated to the warmer and poorer parts of the world. For example: malaria, dengue, Zika, and chikungunya virus.
But global warming and roving mosquitos are rapidly blowing up the traditional boundaries of what counts as “tropical.” A new study in the journal Royal Society Interface finds that many of these diseases can now be transmitted by mosquitoes across most of southern and central Europe, The Guardian reports.
To be clear, the study isn’t just a speculative forecast. For some of these diseases, the shift has already happened.
Take chikungunya. “Up until last year, France had recorded 30-odd cases of chikungunya over the last 10 years or so. [In 2025], they had over 800,” said Steven White, one of the scientists at the UK Centre for Ecology and Hydrology that was behind the new study.
- Disease breakdown: Chikungunya (a particular focus of the new study) is a virus first identified in Tanzania in the 1950s. Its name means “that which bends up,” a nod to the symptomatic contortions caused by terrible joint pain and fever. Although there’s no cure, death is rare, with fewer than 1 in 1,000 perishing from the illness. The real cost is in long-term pain: chronic arthritis that can last for months or years.
One of the study’s most unsettling findings for chikungunya was that the virus can incubate inside the increasingly invasive Asian tiger mosquito at much lower temperatures than previously believed. Specifically, “the study found the cut-off temperature for transmission is 13 degrees C - 14 degrees C,” or about 55 to 57 degrees F.
That dramatically expands the map of where outbreaks are possible, “meaning infections can occur for more than six months of the year in Spain, Portugal, Italy, and Greece, and for three to five months of the year in Belgium, France, Germany, Switzerland, and a dozen other European countries.”
What’s the takeaway?
First, it’s increasingly hard to see the northern spread of these tropical diseases (across North America, too) as anything but inevitable. As winters grow milder and warm seasons stretch longer, the conditions that allow these viruses to circulate are expanding … and exponentially!
I reached out to Flavia Riccardo, an independent infectious diseases researcher at the Italian National Institute of Health. She shared a recent study she co-authored that adds an important nuance. For now, the main risk is not these viruses becoming permanently established in Europe. It is infected travelers bringing them in during mosquito season, and triggering local outbreaks that can flare out of control.
My second takeaway is this: If there’s a morbid upside, it may be that once these diseases begin affecting wealthier countries, they could finally attract the sustained research funding and political urgency they need.
Guinea-Bissau stomps out a controversial vaccine trial
Last week, I mentioned in passing that World Health Organization Director-General Tedros Ghebreyesus publicly condemned a controversial U.S.-funded vaccine study on infants in the West African nation of Guinea-Bissau. Now, the country has shut it down, Reuters reports.
Guinea-Bissau’s foreign minister ultimately said, “It’s not going to happen, period,” after scientists, health bodies, and U.S. lawmakers raised alarms.
The trial, backed by the U.S. Centers for Disease Control and Prevention, would have tested the timing of the hepatitis B vaccine in newborns. Some “critics had said it was being used to test theories linking vaccines to autism,” and others (including the WHO chief) decried it as unethical because only half of infants would receive the life-saving shot at birth.
The threat here is clear: “90% of babies exposed to hepatitis B at birth or in their first year of life develop a chronic infection, and 15% to 25% of these die early of related liver failure or cancer as a result.”
To be perfectly fair to the researchers, “under the [proposed] trial, half the infants would receive [the vaccine] at birth,” and “the remainder at 6 weeks,” which is when infants normally receive the vaccine in the formal health care system in Guinea-Bissau. So the researchers hadn’t planned on taking anything away from vulnerable infants. The African nation “plans to introduce the dose at birth only in 2028.”
Still, at 6 weeks, “many infants whose mothers have hepatitis B are already infected,” and as I wrote last week: It is just hard to imagine a similar trial within the United States surviving legal/ethical challenges.
Magic mushrooms go mainstream
Magic mushrooms are having a bit of a clinical moment.
Compass Pathways, a British pharmaceutical company, announced that its synthetic psilocybin (which is the psychoactive chemical found in magic mushrooms) treatment hit its “major goals” in a large, late-stage trial for hard-to-treat depression, Reuters reports.
The report says that the company now plans to meet with the U.S. Food and Drug Administration and could seek approval for the treatment as early as 2027. (Keep in mind, this would be the first approved psychedelic therapy cleared in the United States.)
What’s my takeaway? Before we all start penciling psychedelics into the next generation of antidepressants, I’d strongly recommend reading this thoughtful essay published in STAT last week.
Erica Rex, a writer who participated in an early magic mushroom trial, warns that the rush to commercialize psychedelics is stripping away the therapy, community, and careful supervision that made those early studies feel safe and transformative. She argues that the drug alone is not the treatment. And profit incentives may directly clash with the slow, human elements that made psychedelic therapy work for her.
A ‘clock’ for Alzheimer’s symptoms
A new study published in the research journal Nature Medicine suggests we may soon be able to do something Alzheimer’s researchers have long dreamed of: Detect Alzheimer’s disease early and estimate when symptoms will begin, the Washington Post reports.
The study describes how to use blood draws to “build a ‘clock’ for Alzheimer’s disease that could roughly predict when symptoms will develop.” The core of the work revolves around tracking the levels of “one specific protein, called p-tau217,” in the blood.
This protein is important, because it is a hallmark sign that Alzheimer’s has started. More specifically, it shows that “clumps of misfolded proteins called amyloid plaques [have] begun to build up in the brain.”
Now just measuring that protein in blood draws isn’t enough on its own.
The bloodwork data has to be fed into a computer model that contains information about the patient, such as their age, which is then used to “forecast symptom onset within a margin of three to four years.”
So, yeah… it’s a wide error range. And practically speaking, this kind of prediction isn’t precise enough yet to guide individual treatment decisions.
But (and here’s the important part!) it could matter enormously for the potential, future use of novel drugs. That’s because two big Alzheimer’s studies underway are testing if newly developed “anti-amyloid” drugs can slow or prevent the disease if they’re given early enough.
If those drugs truly work best early, then knowing when “early” begins would be incredibly important.
The quest for a universal vaccine
I want to tread very, very carefully here. This next story is genuinely fascinating, but I’ve covered enough “breakthroughs” to know how easy it is to get carried away. The bigger the claim, the more skepticism we should hold.
The journal Science has just published a paper describing a provocative new approach to developing a “universal vaccine,” the BBC reports. That is, a vaccine that doesn’t just target one virus, but puts the entire immune system on high alert against many.
The paper is not theoretical. Stanford University scientists developed a nasal spray vaccine that they tested on mice against infections that attack the lungs. The end result was a “three-month effect” in which the mice’s immune systems were in a “heightened state of readiness” that “led to a 100- to -1,000-fold reduction in viruses getting through the lungs and into the body.”
This included effective immunity against a medley of cold and flu viruses, among other would-be invaders.
That is big news! So what’s the actual science here? To understand it, it helps to step back and look at what traditional vaccines are actually designed to do.
Traditional vaccines all use different strategies to teach the immune system to recognize a specific virus or bacteria. This is done by either by exposing the body to a weakened, dead, or fragmented germ … or by delivering instructions for the body to make a harmless piece of it (this last one is the new mRNA method, developed during the Covid-19 pandemic.)
This even newer approach is totally different. Instead of teaching the immune system to identify attackers, the vaccine artificially mimics the signals “immune cells [use to] communicate with each other” in the midst of an infection. Normally, when an infection begins, immune cells send out chemical signals that trigger a system-wide defensive response. And when on high alert, immune cells become more active and better able to contain invading viruses or bacteria.
This vaccine recreated that early alarm. It did this by introducing a molecule that flips the sensors inside some immune cells, pushing them into that heightened state of readiness.
Yes, it absolutely does sound like an incredible breakthrough. So … let’s move on to my beloved caveats.
First: This has not been tested in humans. It worked on mice, which is not nothing, but many, many fascinating mouse studies have failed to translate into people.
Second: The researchers now have to run the clinical trial gauntlet. That starts with Phase 1 trial to test safety, Phase 2 to figure out dosing and immune response, and Phase 3 to see whether it actually works in large numbers of people. Historically, only about 10% of drugs that start these trials end as an approved drug. Most are found to be unsafe or ineffective. Even at Phase 3, roughly half still fail.
Still, it’s promising.
I’ll see you next week!
William
William Herkewitz is a reporter covering global public health for Healthbeat. He is based in Nairobi. Contact William at wherkewitz@healthbeat.org.